Medication alone is rarely the complete answer for individuals with bipolar disorder. Responses are incomplete, prevention is imperfect, lingering symptoms remain and adherence to treatment is often a challenge. Substance use, inadequate and irregular sleep schedules, fluctuations in activity, and poor regulation of emotional stimuli can also contribute to limiting the effectiveness of medications. For these and other reasons, psychological therapies have been investigated as adjuncts in the overall management of this illness.
History and Development of Psychoeducation
The first psychological efforts to address bipolar disorders were intensive, psychoanalytic therapies conducted during the first half of the 20th century. Occurring at a time when there were no other empirically proven treatments, these psychoanalytic therapies that were designed for more common emotional problems did not show promise in altering the course of manic-depressive illness. Following this, cognitive behavioral therapy and family focused therapy were two of the first, standardized psychological interventions evaluated in the treatment of bipolar disorders.
Psychoeducational therapy for bipolar disorders arose in the late 1980’s. It occurred in reaction to the traditional medical model prevalent prior to that time. That medical model was characterized as paternalistic and biomedical, viewing illness as the sole cause of suffering and doctors and their medications as the sole source of treatment. The patient’s understanding of their condition was not seen as important and patients were not active participants in their treatment. Enter psychoeducation.
Psychoeducation was a radical break from the medical authoritarianism of the early 20th century. Based on the premise that knowledge is power, its goal was to provide information to patients about their illness. Early reports from the Netherlands suggested that this approach could improve self-confidence and lessen the isolation and stigma that mental illness so often confers. Matters that we take for granted today.
A Current Model of Psychoeducation
These early efforts paved the way for later, more refined psychoeducational therapies. Combining information provision with elements of proactive self-management and social support, Colom and colleagues in Barcelona developed the first, modern psychoeducational therapy for bipolar disorders 1. It consisted of 21 group sessions, each focusing on one of five major areas:
Awareness of the disorder
Medication adherence
Avoiding substance abuse
Early detection of new episodes
Regular habits and stress mgmt.
Here is a list of the 21 topics covered in each of the above five areas:

Research Findings
Designed as a maintenance treatment to prevent relapse among stable, euthymic patients, the first study of this modality was wildly successful, showing dramatically reduced relapse rates for manic, depressive and mixed mood episodes over the two-year time period of the study (see graph below).
A follow-up study on the same cohort of subjects, tested three years later showed that the benefits not only persisted but – in some cases (e.g., manic relapse) – had increased over time 2. Incredible results!
As a consequence of these foundational reports and some other replication studies, psychoeducation was adopted by several international treatment guidelines as a first-line, adjunctive treatment for all individuals with bipolar disorder who were in stable remission. But then, as always, the story got a little more complicated.
In 2015, Kirsten Bond and colleagues from the UK, conducted a careful systematic review of all studies done on psychoeducation 3. A systematic review is a prescribed, formal method of scouring the entire scientific literature on all studies in a given area. It is designed to be thorough, clear, transparent and objective, attempting to avoid the biases that can plague individual studies. Combing through an initial search of almost 1600 articles, the authors found only 8 that met their strict inclusion criteria. The upshot? When pooling the results of these eight studies, they confirmed that psychoeducation significantly reduced relapse into any mood episode, especially manic relapse. Their finding on prevention of depressive relapse were more equivocal and were only significant when examining group-based (vs. individual) psychoeducation. Two more caveats. First, they noted that there was considerable variability in the treatment formats used in the studies; some used individual psychoeducation, others used group. The length of treatments varied between as few as 2 and as many as 21 sessions. This heterogeneity introduced uncertainty to the overall findings. Second, the results from the initial studies by Colom’s group in Barcelona were outliers; they were much more significant than all the other studies. When those were removed, the efficacy of psychoeducation in the remaining studies was cut in half. Further sobering news followed.
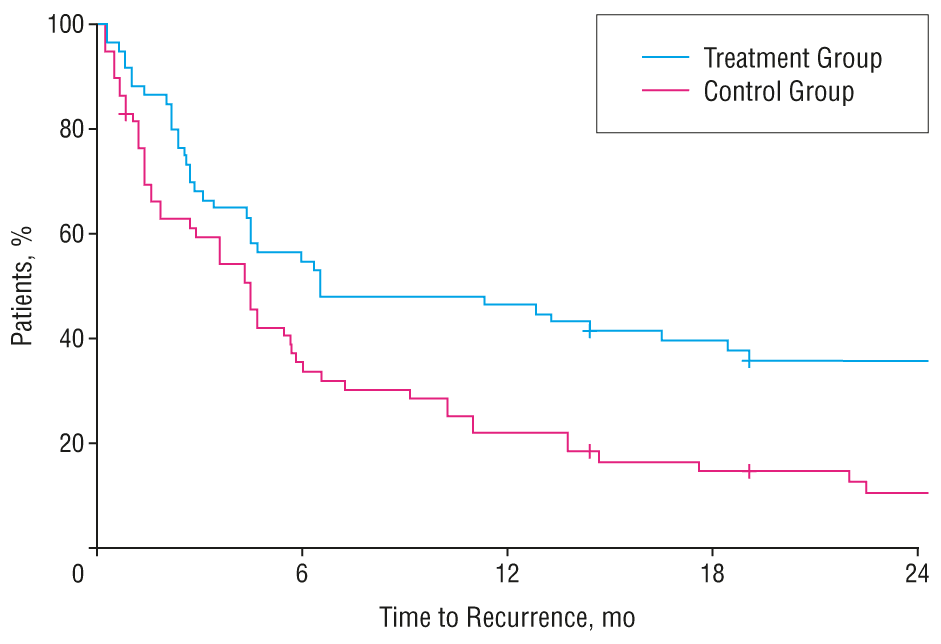
Prompted by the caution of this systematic review and a relative absence of independently conducted replication research, Richard Morriss and colleagues designed a careful, randomized, single-blind study of psychoeducation vs unstructured peer support groups 4. As with all research in this area, the psychoeducation and control groups were adjunctive to standard medication therapy. Their design, however, differed in two significant respects from the original research of the Colom group: First, instead of requiring six months of mood stability (euthymia), they required only 4 weeks; second, while Colom excluded patients with any comorbid disorders (eg, anxiety problems, substance abuse, etc..), these authors allowed almost anyone to enter their study. This creates more of a real-world examination of the treatment. Apart from these distinct inclusion and exclusion criteria, the treatment was exactly the same as the Colom group: 21 group sessions. The primary outcome measured was time to relapse over the almost two years of the study. The main results are shown below:

The graph shows survival curves of the two groups, representing the percentage of each group that “survived” or avoided relapse over the 92 weeks of the study. As you can see, the curves are almost identical, indicating no significant difference between the psychoeducation and control arms of the study. Yikes! How do we explain the differences between the initial, dramatically positive results for this intervention and the later, more cautious systematic review and this recent, negative study? And what does this mean for the status of this first-line psychological treatment for bipolar disorders?
Synthesis and Conclusion
We suggest that the way to reconcile these contradictory findings lies in the different entry criteria and cohorts used in the initial vs. the later studies. Colom’s group set a very high bar for participation in their research: subjects needed to be euthymic for six months and free of other major psychiatric disorders. This creates an ultra-rarefied cohort, one that would not generalize well to the real world where patients typically have several disorders at once and are rarely free of symptoms for extended periods of time. If this difference accounts for the disparate findings, this suggests that psychoeducation might be more useful early in the course of their illness and in those patients without significant comorbidity. Here’s our take home on this.
Psychoeducation is an intervention designed to help individuals with bipolar disorders better understand their illness and their ability to manage it.
The weight of research on psychoeducation supports a maintenance effect of preventing episode relapse.
This relapse prevention effect is probably more pronounced among patients who have not had high numbers of prior episodes or multiple other existing mental health disorders.
While perhaps not the glowing success that the foundational studies suggested, in terms of providing patients with a coherent way of understanding and managing the tumultuous course of their mood states, psychoeducation remains the best game in town. We believe it should remain as part of the ‘core curriculum’ of all treatment efforts.
John Gottlieb
1. Colom F, Vieta E, Martinez-Aran A, et al. A randomized trial on the efficacy of group psychoeducation in the prophylaxis of recurrences in bipolar patients whose disease is in remission.[see comment]. Arch Gen Psychiatry. 2003;60(4):402-407.
2. Colom F, Vieta E, Sanchez-Moreno J, et al. Group psychoeducation for stabilised bipolar disorders: 5-year outcome of a randomised clinical trial. Br J Psychiatry. 2009;194(3):260-265.
3. Bond K, Anderson IM. Psychoeducation for relapse prevention in bipolar disorder: a systematic review of efficacy in randomized controlled trials. Bipolar Disord. 2015;17(4):349-362.
4. Morriss R, Lobban F, Riste L, et al. Clinical effectiveness and acceptability of structured group psychoeducation versus optimised unstructured peer support for patients with remitted bipolar disorder (PARADES): a pragmatic, multicentre, observer-blind, randomised controlled superiority trial. The lancet Psychiatry. 2016;3(11):1029-1038.
